Blog
Home Infusion and the Rise of Virtual Care

At first blush, the specialized delivery of home infusion may not seem to lend itself to virtual care. Yet we think all elements of home care are about to permanently change when it comes to this subject, thrust into the spotlight due to COVID-19.
“Virtual” extends to phone calls, recorded video, live video conferences, remote patient monitoring, and wearable technology. When it comes to video, while there is no substitute for in-person interactions, the need for physical distancing has shown society that we can do a lot more things virtually than we might have imagined. And we can stay connected much easier and at any time.
How will this evolution impact home infusion providers? We believe that supervisory visits and assessments that can be virtual will permanently change the industry. In the here and now, it’s been compelled by COVID-19 and in the future, it will be compelled by efficiency.
It’s up to agencies to determine their comfort level with virtual care, but the possibilities are real. Outside of administering medication, how many visits by nurses are more about monitoring patient progress or collecting vitals? Can this burden be shifted to clients, enabling them to take greater control of self-managing their care? With the right tools and support, many clients can be responsible for some documentation.
In the same vein, family caregivers can become more sophisticated members of the healthcare team. They can be coached through some interventions, on how to capture vitals and monitor their loved ones from afar. We have seen a clue at AlayaCare as to the acceptance of this elevated role: our Family Portal software accelerated in adoption after COVID-19 struck. Through the portal, everyone has visibility into care planning, preventing miscommunication among the often many loved ones invested in a client’s care.
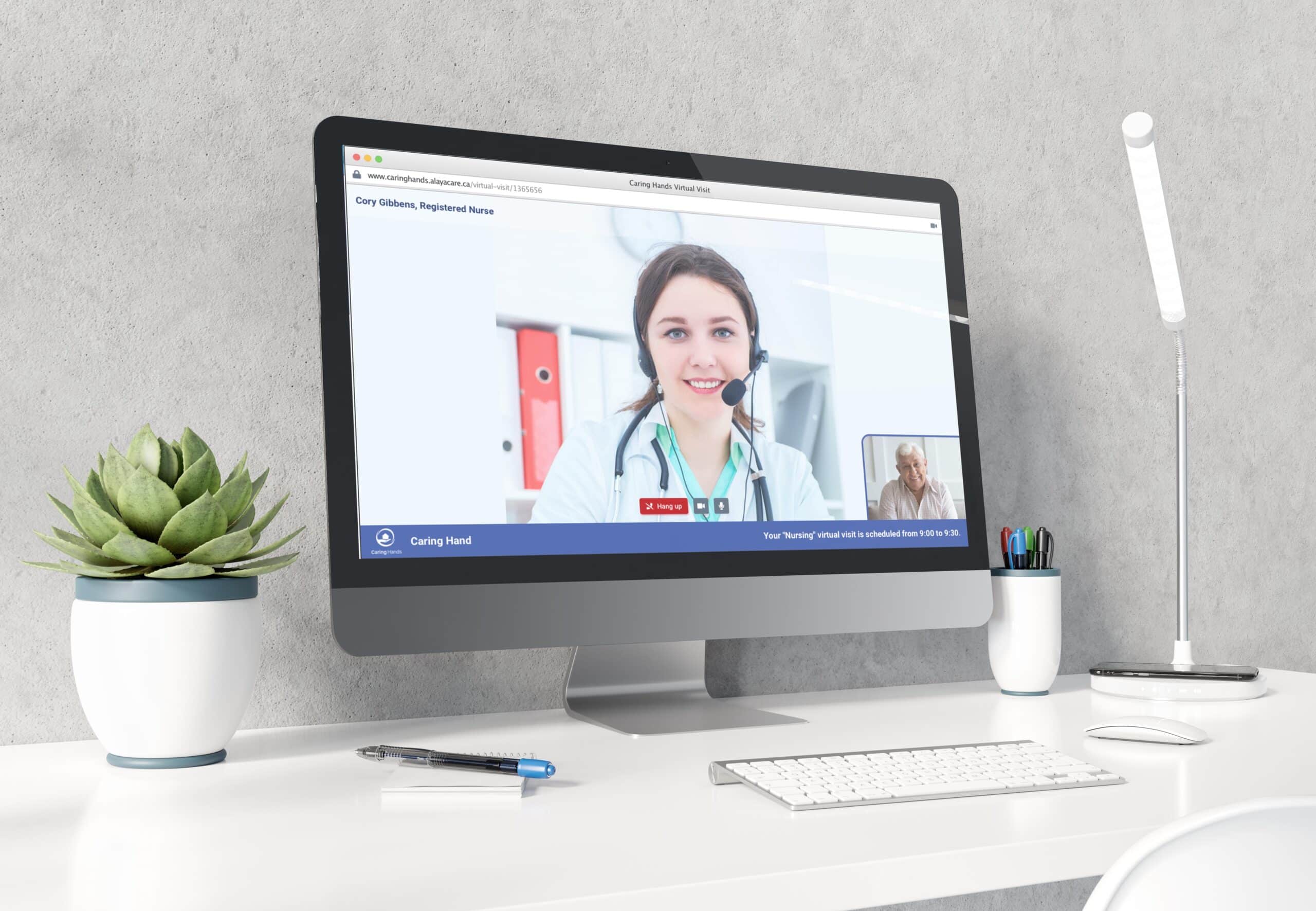
Then we come to the actual virtual appointments with skilled staff. The AlayaCare virtual care suite allows nurses to adjust the service code on any visit in the schedule to be conducted virtually. An email is sent to the client with one secure link that creates a virtual interaction within the system. Nurses or caregivers can do real-time charting in the app just as they might with an in-person visit. Instead of performing, say, four visits in one day, that nurse could do eight virtually. This newfound capacity is a surplus of what was a scarce resource only months ago.
Another concept abetted by software is risk stratification: tools that can help clinicians direct their attention toward higher-risk clients. Based on diagnoses, demographics, and vital signs, a risk profile for each client can be aggregated. In this manner, nurses can devote more time to higher-risk clients, or those whose status may be deteriorating – with easy virtual visits or in-home appointments.
If you are a home infusion agency looking for a home infusion billing software solution, you have come to the right place.