Blog
AlayaCare + Waystar = Deep Integration, Unparalleled Benefits

We were thrilled to recently announce our partnership with Waystar — the top medical billing clearinghouse in the U.S. and an exceptionally powerful tool for our Medicaid clients looking for a turnkey solution to connect care providers, insurers and other payers.
AlayaCare’s integration with Waystar is deeper than any other home care software provider and, in fact, is the only software to date that has harmonized with Waystar on an individual visit-by-visit basis.
This integration offers an unparalleled tool for agencies to not only improve efficiency by automating important (often time-consuming) tasks but enjoy greater transparency into the status of Medicaid claims with real-time updates embedded within AlayaCare. Thanks to built-in quality control, agencies can have peace of mind knowing Waystar protects against denials to the point that 97 of every 100 claims are approved and paid. For more details on how technology can relieve the pain of billing in home care — including with Medicaid clients, be sure to check out our most recent in-depth article on the subject here.
The Waystar collaboration is the latest endeavor in our ongoing mission to help agencies stay focused on their clients by building thoughtful, simple solutions to address important yet often cumbersome processes — such as billing.
Waystar: No. 1 ranked clearinghouse in the U.S.
So who is Waystar, and why did we choose to partner with them?
Waystar is an industry-leading U.S. medical billing clearinghouse, a bridge connecting care providers and insurers and other payers. Powered by 800 employees across the United States, Waystar serves more than 450,000 providers, assimilates more than 750 hospitals and health systems, and connects to 5,000 payers and health plans.
Waystar’s exceptional reach is the result of strategic growth moves, beginning with the November 2017 merger between Navicure and ZirMed. Not long after, Waystar acquired Connance, another revenue recycle technology company.
Its highly-rated revenue cycle management technology proactively ensures that providers such as home care agencies are reimbursed in a timely manner. The technology extends across every type of care setting. To date, it has processed over two billion transactions and integrated 530 types of software.
Like AlayaCare, Waystar employs a variety of tools that automate previously manual processes, using predictive analytics to identify missing charges. It is customizable to each organization, offering a personalized experienced, intuitive navigation and streamlined workflow.
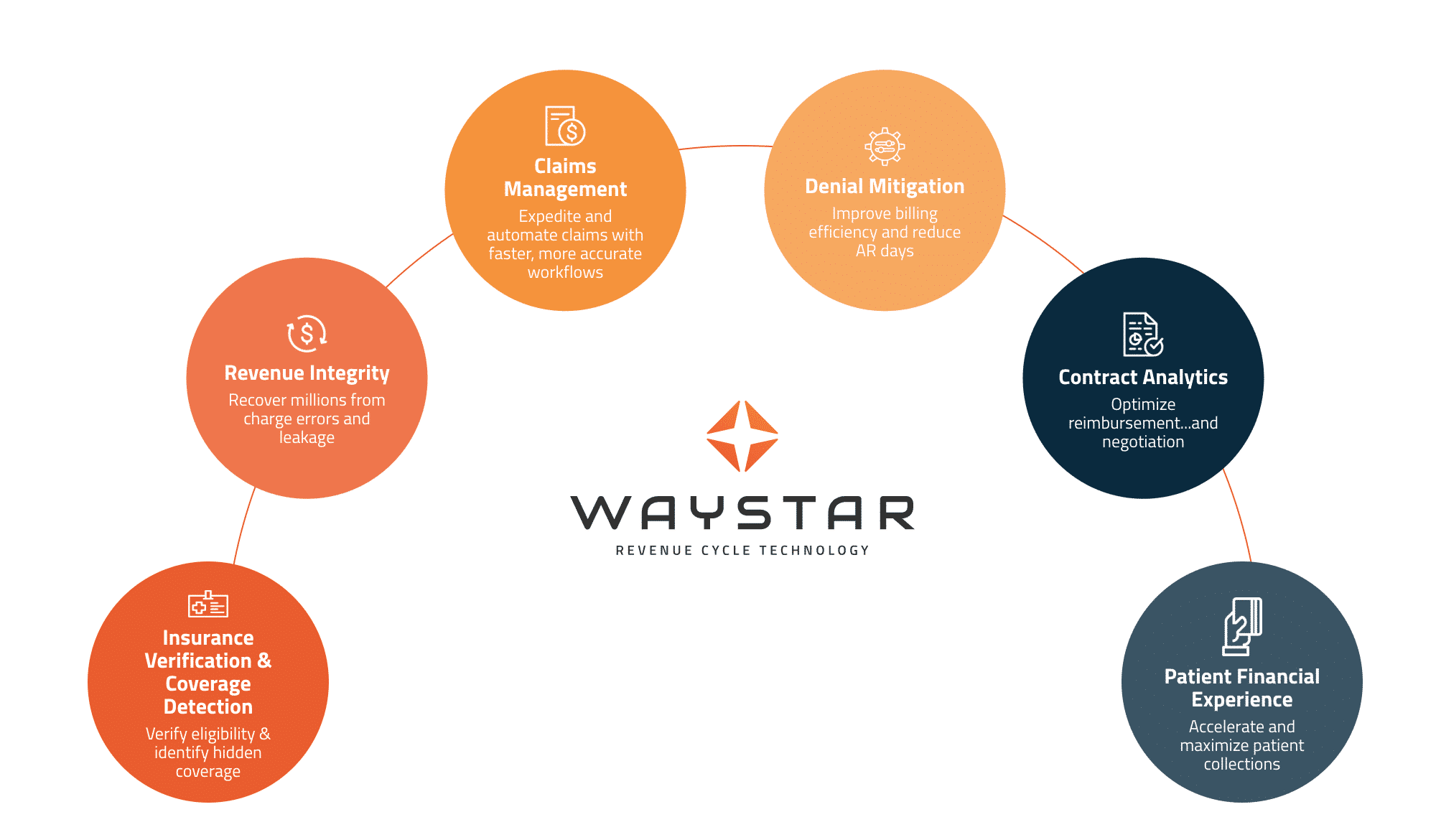
Here’s a recap of the key benefits you can expect by tapping into this powerful integration with AlayaCare:
Revenue cycle management: Waystar-AlayaCare reimbursement solutions automates many tasks that would otherwise drain productivity. These solutions apply a consistent, revenue-generating approach to each client’s unique revenue cycle management (RCM) processes for maximum efficiency.
Seamless transactions: This integration allows AlayaCare to transmit and receive a variety of claims, payments, eligibility inquiries and other healthcare transactions using established technologies and methods — including X12 files, APIs, Flat Files, FTP, and Encryption (i.e. PGP).
Maximum Reimbursement: RCM tools for billing services provide real-time eligibility information that can also identify hidden coverage.
{{cta(‘5060a845-1de3-4210-a74f-01975659b845’)}}
Contact us to find out how you can start leveraging the benefits of AlayaCare and Waystar for your business.